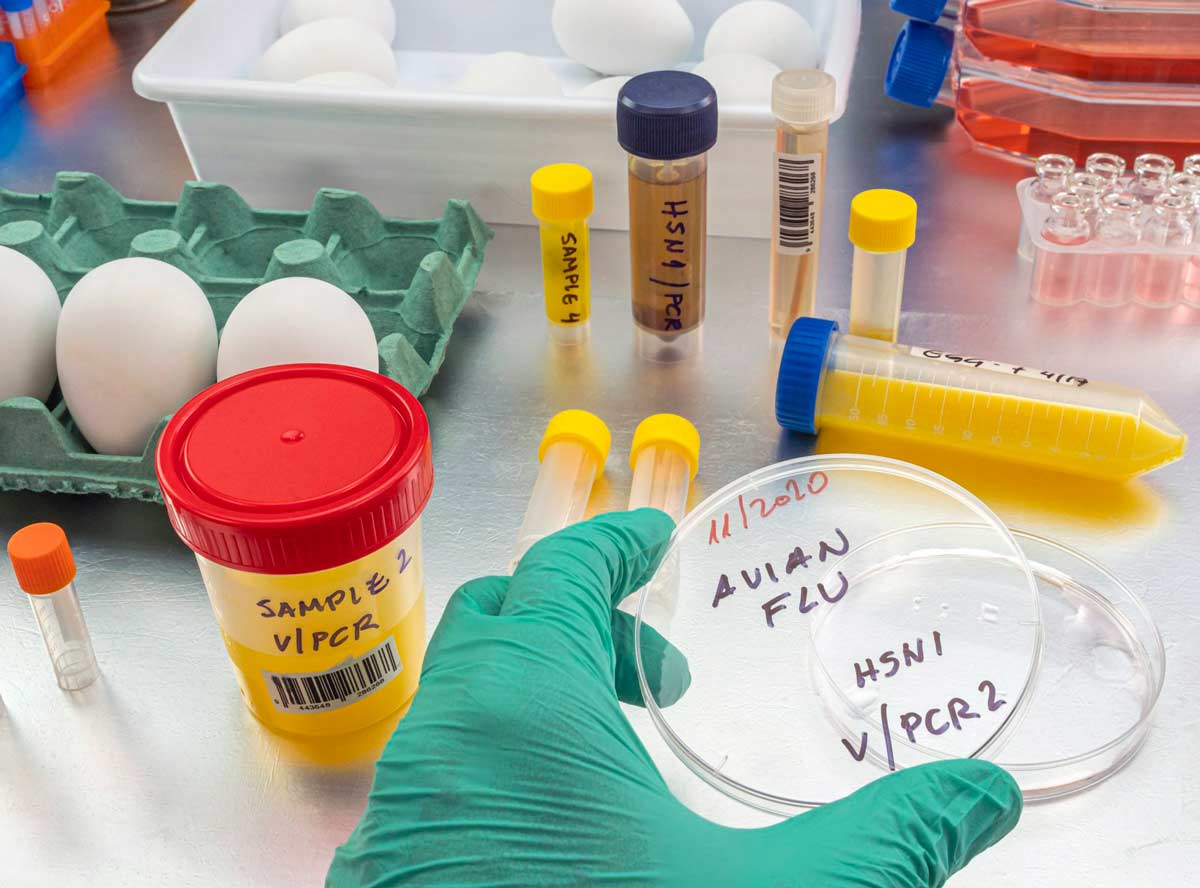
Avian flu has infected dairy cows in more than a dozen US states – a microbiologist explains how the virus is spreading
The H5N1 virus has infected about 900 people since 2003, and more than half of them died. But so far there is no evidence of human-to-human transmission.
- 29 August 2024
- 5 min read
- by The Conversation

The current strain of avian flu, H5N1, is responsible for the culling of millions of domestic birds and has sickened more than a dozen farmworkers in 2024, most recently in Colorado.
The Conversation U.S. asked immunologist and microbiologist Jenna Guthmiller from the University of Colorado Anschutz Medical Campus to explain the historical roots of H5N1, its mode of transmission and how to avoid coming into contact with it.
What is H5N1?
H5N1 is a subtype of influenza A viruses. Other commonly known influenza A virus subtypes include H1N1 and H3N2, which cause seasonal outbreaks in humans.
Unlike H1N1 and H3N2, H5N1 largely infects wild birds, with waterfowl such as ducks and geese being the natural reservoirs for H5N1 viruses. Most H5N1 viruses are highly pathogenic avian influenza, meaning spillovers into other bird populations can lead to high mortality rates, including domesticated poultry.
H5N1 viruses were first identified in 1959 due to an outbreak in domesticated chickens in Scotland. In 1996, waterfowl were identified as the natural reservoir for H5N1.
Since its identification, H5N1 viruses have led to four major outbreaks: in 1997, 2003-2005, 2015 and 2021-to-present. The outbreaks in 1997 and 2003-2005 led to substantial spillover to humans.
Since 2003, nearly 900 H5N1 infections in humans have been recorded. Of those infections, more than half were fatal.
Where did H5N1 originate?
The current outbreak of H5N1 started in late 2021 and derives from the virus that caused a major outbreak in 2015.
Since 2021, H5N1 strains have spread to six continents by migratory birds. Spillover to domestic poultry has led to the culling of millions of domestic birds
Researchers have documented the current H5N1 strain in numerous mammals, with it largely affecting aquatic mammals like seals and scavenger mammals. Sporadic spillover to domestic mammals has been recorded, including to minks, goats and alpacas.
In March 2024, the U.S. Department of Agriculture reported an outbreak of H5N1 in lactating dairy cows. As of Aug. 27, 192 herds in 13 states have been confirmed H5N1 positive.
Dairy cow-associated H5N1 viruses have since jumped back into wild birds, and recent outbreaks in domestic poultry resembled H5N1 in dairy cows. Between May and July 2024, 13 confirmed H5N1 infections have occurred in humans, with all cases directly linked to dairy farms and poultry culling.
Why did the avian flu become more widespread?
It is unclear why H5N1 has become such a widespread problem. H5N1, like all influenza viruses, rapidly mutates to infect new hosts. However, H5N1 has several features that could increase its host range.
First, H5N1 viruses use a protein called hemagglutinin that allows H5N1 to infect with new hosts.
Second, my research group identified a mutation in H5N1 viruses causing the dairy cow outbreak that allows hemagglutinin to bind to its receptor more efficiently.
Lastly, H5N1 viruses are mutating genes associated with replication and immune evasion that are known to increase the infection of mammals.
Together, these factors could heighten H5N1 transmission and increase H5N1 spillover to mammals.
How is the strain transmitted to dairy cattle?
H5N1 viruses are largely causing infections in the mammary glands of cattle rather than the respiratory tract, which is the main site of infection for other influenza viruses in mammals. Recent studies have shown that the mammary tissue has receptors for H5N1, which could make this tissue susceptible to infection.
Since the infection is largely restricted to the mammary glands, researchers believe that H5N1 is being transmitted to cows by contaminated milk equipment, particularly the milking apparatus that attaches to the cow udders. Transmission across farms is due to infected cattle movement and shared equipment and personnel across dairy farms.
To reduce transmission, in April 2024, the USDA put in testing requirements for when cows are transported across state lines. In addition, Colorado, the state with the greatest number of positive herds, requires weekly testing on farms to identify infected herds.
What are the risks to people and other animals?
H5N1 does not pose a risk to the general public, as this virus is not known to transmit between people. As all known cases were those with direct contact with infected animals, people with occupational exposure to H5N1-infected cows and poultry continue to be at the greatest risk of infection.
People with occupational hazards should be aware of the H5N1 symptoms – similar to those of a cold – such as congestion, sore throat and fatigue, as well as conjunctivitis, more commonly known as pink eye. For more information, see the Centers for Disease Control and Prevention’s webpage on avian influenza in people.
Domestic and wild animals near dairy farms are at high risk of infection. Particularly, barn cats that have been fed raw milk have been reported dead on dairy farms with infected cows, with these animals coming back positive for H5N1.
In addition, spillover of H5N1 to other domesticated farm animals near infected dairy cows has been recorded.
What are the best ways to keep farm workers safe?
Using personal protective equipment, such as goggles and gloves, remains the best way to prevent the transmission of H5N1 to humans and from humans back to animals. People working around poultry or dairy cattle should also be aware of biosecurity measures, such as not wearing the same clothes and boots when traveling from one farm to another.
Have you read?
Is drinking dairy milk a concern?
As long as you are consuming pasteurized milk products, there are no concerns for infections in humans. Pasteurization is very effective at killing any H5N1 virus that ends up in milk.
People should avoid raw or unpasteurized milk, as H5N1 virus has been found at very high levels in raw milk.![]()
More from The Conversation
Recommended for you